 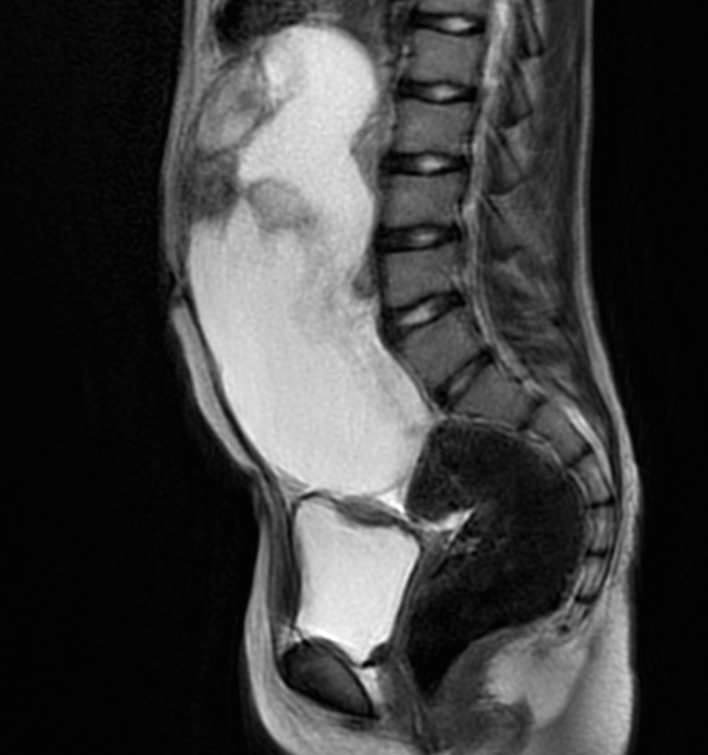
All of this can be done at laparoscopic surgery.Īs with dermoid cysts, they tend to grow progressively, but unlike dermoid cysts, they can be partly shrunk with additional medication. The anatomy must be restored first and foremost, and then the cysts removed by peeling the capsule from the inside of the stretched ovarian cortex. The underlying attachments is the most crucial part of any surgery to remove these endometriomas. As is always the case with this pathology, there is nothing romantic about their attachments to various other organs (bowel, vagina, uterus, pelvic walls, even bladder). These cysts can be from 3cm to 20cm in diameter and once larger than 10cm, usually join with the other ovary to produce a phenomenon known as ‘kissing ovaries’. Fertility can be easily retained, with no loss of future potential. With careful attention to detail, the majority of the ovarian tissue (therefore egg bearing cortex, ovarian reserve) can be preserved. They form within the ovary and so need to be carefully removed, much like peeling an orange or a grapefruit. They are relatively easily removed at laparoscopic surgery, though once their size exceeds 10cm they are technically much more difficult to remove. They can sometimes be confused on scan with endometriomas, or even haemorrhagic cysts, but the giveaway is that they most often contain fat cells and/or bone fragments or teeth.ĭermoid cysts grow slowly but progressively. Most dermoid cysts are found incidentally. Much less common is the immature teratoma, which is a relatively aggressive type of ovarian cancer. The alternate name for these is mature teratoma, usually seen in women aged 15 to 45. Almost all are benign, though only histological analysis after removal can confirm the exact nature of a dermoid cyst. 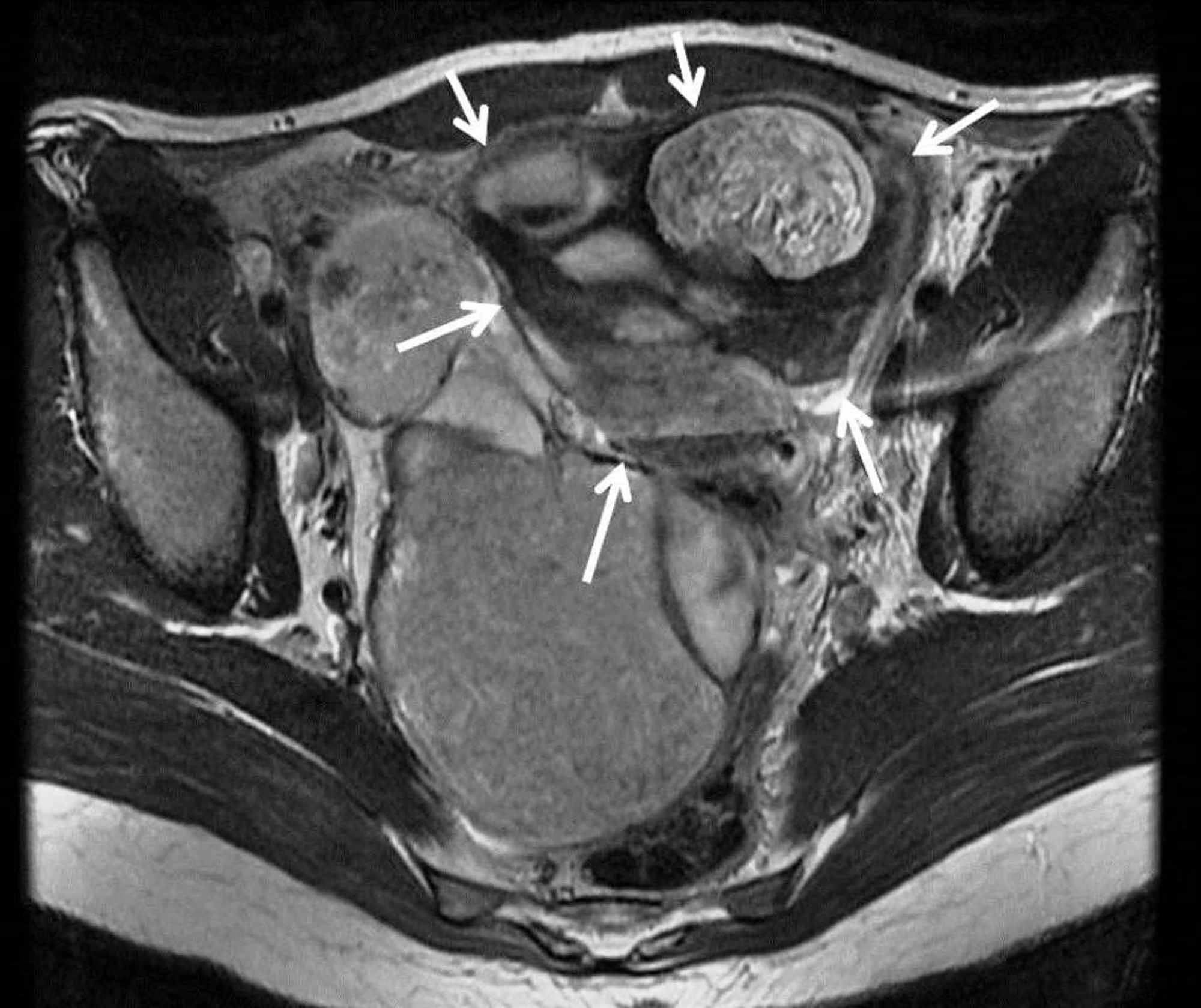
These contain skin-derived elements, so unusually may have teeth, bone, gland cells, hair and even brain tissue. There are unusual variations of benign cysts, with three stand-out examples being dermoid cysts, endometrioma cysts (aka chocolate cysts) and benign serous/mucinous ovarian tumours. That is, they do not contain unusual solid and cystic spaces, have a smooth internal and external wall and a normal blood supply, and often contain fluid that has the same ultrasound echo pattern (homogeneity). The vast majority of cysts that Dr Gordon sees are benign. Pathological cysts: structures that continue to grow independently of the menstrual cycle they can be further classified into sub-groups:.Physiological cysts: ‘fluid filled spaces’ that occur with ovulation, such as follicular and luteal phase cysts (the fundamental characteristic of physiological cysts is that they occur, then are resorbed within one or two menstrual cycles).Ovarian cysts can be divided into two main categories: 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
